Improvement Project Progress on a 1 to 5 scale—Part 2
In Part 1 of this post, I introduced the 1-5 Project Scale developed by colleagues at the Institute for Healthcare Improvement (www.ihi.org). The scale is part of the innovation known as the Breakthrough Series collaborative—a method to accelerate improvement in a community of organizations. I outlined the difference between testing a change and implementing a change.
In this post, I connect level 3 of the 1-5 scale to a pair of fundamental management methods critical to implementation.
Application in an Oral Health Improvement Collaborative
I serve as an Improvement Advisor to a collaborative with twenty-six dental groups, from federally qualified community health centers here in the United States. The collaborative aims to improve oral health over 12 months for children and adolescents; we’re using a set of changes in work practices and patient engagement developed in a previous pilot project.
On a call last week with one of the groups, the lead dentist for the organization’s improvement team was most concerned about holding onto gains from initial testing of changes; he said staff were asking if "we still have to keep doing these new things.”
That question is at the heart of the distinction between testing and implementation discussed in the previous post. How will you keep useful changes in place for every patient, every time?
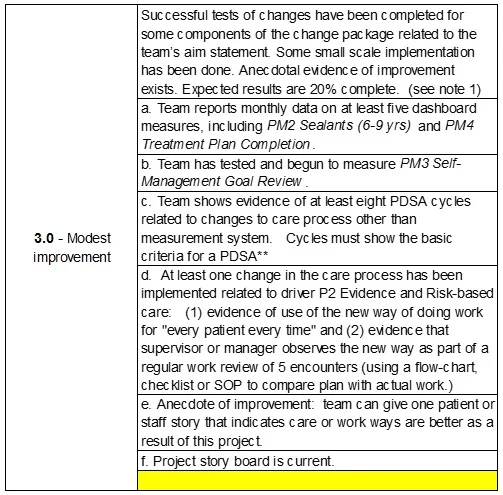
We introduce an initial answer in part 3d of our Collaborative’s project progress scale. “Small scale implementation” is defined this way:
d. At least one change in the care process has been implemented related to driver P2 Evidence and Risk-based care: (1) evidence of use of the new way of doing work for ‘every patient every time’ and (2) evidence that supervisor or manager observes the new way as part of a regular work review of 5 encounters (using a flow-chart, checklist or SOP to compare plan with actual work.)
Remember the definition of implementation: To make a change part of regular work in a system.
How will supervisors get evidence that a change has been implemented? For example, how will supervisors know if their clinic has implemented changes like assessing every child’s risk for dental caries or assuring that at-risk 6-9 year olds have appropriate dental sealants?
Look at item (2)--go observe five encounters or treatments or patients under care.
Can people do the work as planned? If you observe 5 out of 5 work cycles that follow the plan, that's pretty good evidence. We ask the supervisor to have a standard document in hand--a flow-chart, a check-list or a written SOP--to take observation notes, to make it clear how well the actual work matches the planned work.
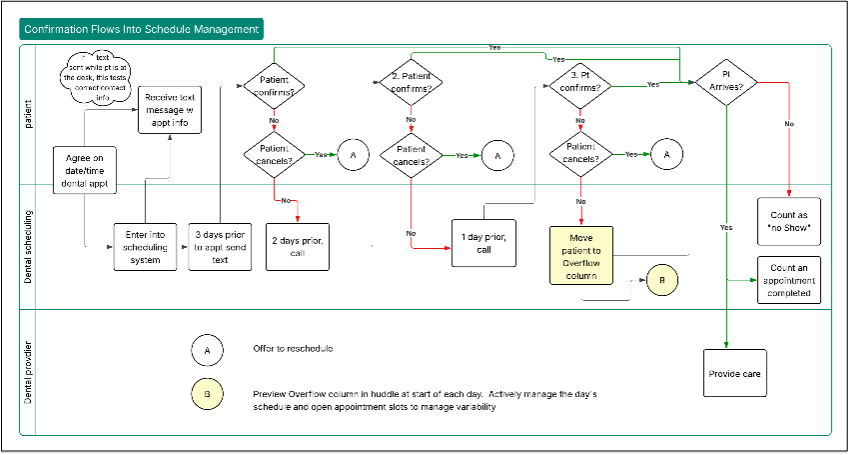
There's another management tool that the dental clinics have already tested: a daily huddle by care teams. The daily huddle is a key way to reinforce that "we're still doing these things."
When the care team huddles, it looks ahead at the patients for the day. It gives them a couple of minutes to consider the patients in need of sealants, risk assessment or the other changes being implemented. The desired changes are built into a quick review of work for the day; the huddle gives a chance for the team to identify what’s needed to be successful in carrying out their standard work.
In the daily huddle, you can reserve a minute or two to look back at the previous day, too. Are there any things that got missed on risk assessment, sealants, or other implemented changes that you can do better today and prevent misses from recurring tomorrow? This review is a robust source of maintenance items, the things to fix to make it easier for the supervisor and care team to assure the changes are indeed part of regular work in the clinic.
Note: Daily huddles and direct observation of work flow are two elements of a management system to sustain improvements, discussed in this post and outlined in the IHI whitepaper, Sustaining Improvement Scoville R, Little K, Rakover J, Luther K, Mate K. Sustaining Improvement. IHI White Paper. Cambridge, Massachusetts: Institute for Healthcare Improvement; 2016, http://www.ihi.org/resources/Pages/IHIWhitePapers/Sustaining-Improvement.aspx.)